For more than 75 years, chemotherapy has been the standard of care for cancer treatment around the world. While this class of drugs has extended and saved many lives, chemotherapies lack the ability to specifically target cancer cells, making them less effective and more toxic than desirable.
Newer classes of drugs that effectively target cancer cells – or mutations within these cells – are radically transforming the treatment of many cancers. Rather than indiscriminately killing both healthy and cancerous cells, these therapies interfere with particular molecular processes that are unique to cancer cells. The identification of new molecular targets for these precision medicine therapies is an important and ongoing need in cancer research.
Currently, most researchers focus on identifying and developing drugs to directly target cancer-specific alterations (certain mutations or overexpressed genes) that drive the cancer. However, many key cancer-specific alterations are not directly “druggable.” Consequently, cancer researchers are now trying to identify alternative processes that the cancer cell depends on for survival and target those processes instead. One of these alternative processes is called “synthetic lethality.” In a cancer cell, if a particular gene is impaired by a mutation, there is an increased and unique dependency on a second gene for cell survival – this second gene is known as the synthetic lethal (SL) partner of the mutation. A defect in both genes can lead to cell death. In other words, targeting the SL partner can cause death for the cancer cells carrying the mutation, while allowing the non-cancerous cells to survive. As a result, SL partners of cancer mutations are generating great interest as pharmacological targets. However, their identification by traditional cell-screening methods such as shRNA and CRISPR has been challenging.
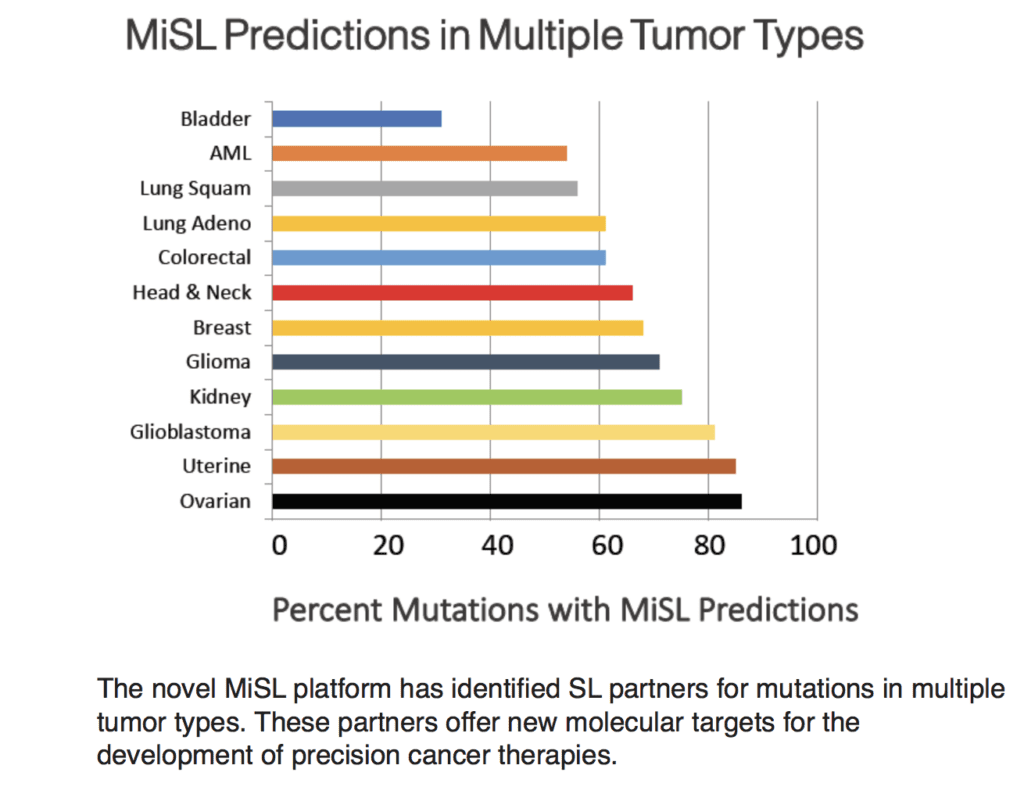
Our team at SRI International has a proprietary platform that overcomes the limitations of the screening-based approaches for target discovery. This platform utilizes a novel computational algorithm called Mining Synthetic Lethals (MiSL) to identify potential drug targets and then validates these targets in in vitro and in vivo models. MiSL identifies the targets by identifying SL relationships within primary human tumor genomes. Because it uses pan-cancer, primary human tumor data rather than artificial models with cell lines (which can change over time, may not be representative and may lack important mutations), MiSL offers several advantages over predecessor discovery platforms.
MiSL has identified valid SL partners in multiple tumor types, including acute myeloid leukemia and kidney cancer. Most recently, my SRI colleagues, Lidia Sambucetti and Yihui Shi, and I used this proprietary, precision cancer therapy platform to identify new molecular targets for the treatment of triple-negative breast cancer (TNBC), an aggressive and particularly difficult-to-treat form of the disease.
The BRCA1 gene is mutated in about 15 to 20 percent of TNBCs, making this cancer type a likely suspect for actionable SL partners. Using MiSL, we were able to identify and predict 22 SL partners of the BRCA1 mutation in TNBC, including XRCC6. We then tested the prediction that XRCC6 is an SL partner of BRCA1 in TNBC by examining the effect of inhibiting this gene in BRCA1 -mutated TNBC cells. XRCC6 “knockdown” increased TNBC cell death by more than 37 percent and reduced cell viability by 50 percent as compared to controls. We are currently testing other SL partners predicted by MiSL for the BRCA1 mutation.
I was honored to present this discovery at the 2018 American Association for Cancer Research (AACR) Annual Meeting, because it opens the door for new, much-needed options to treat BRCA1- related breast cancers, as well as new disease prevention strategies for individuals with inherited BRCA1 mutations.