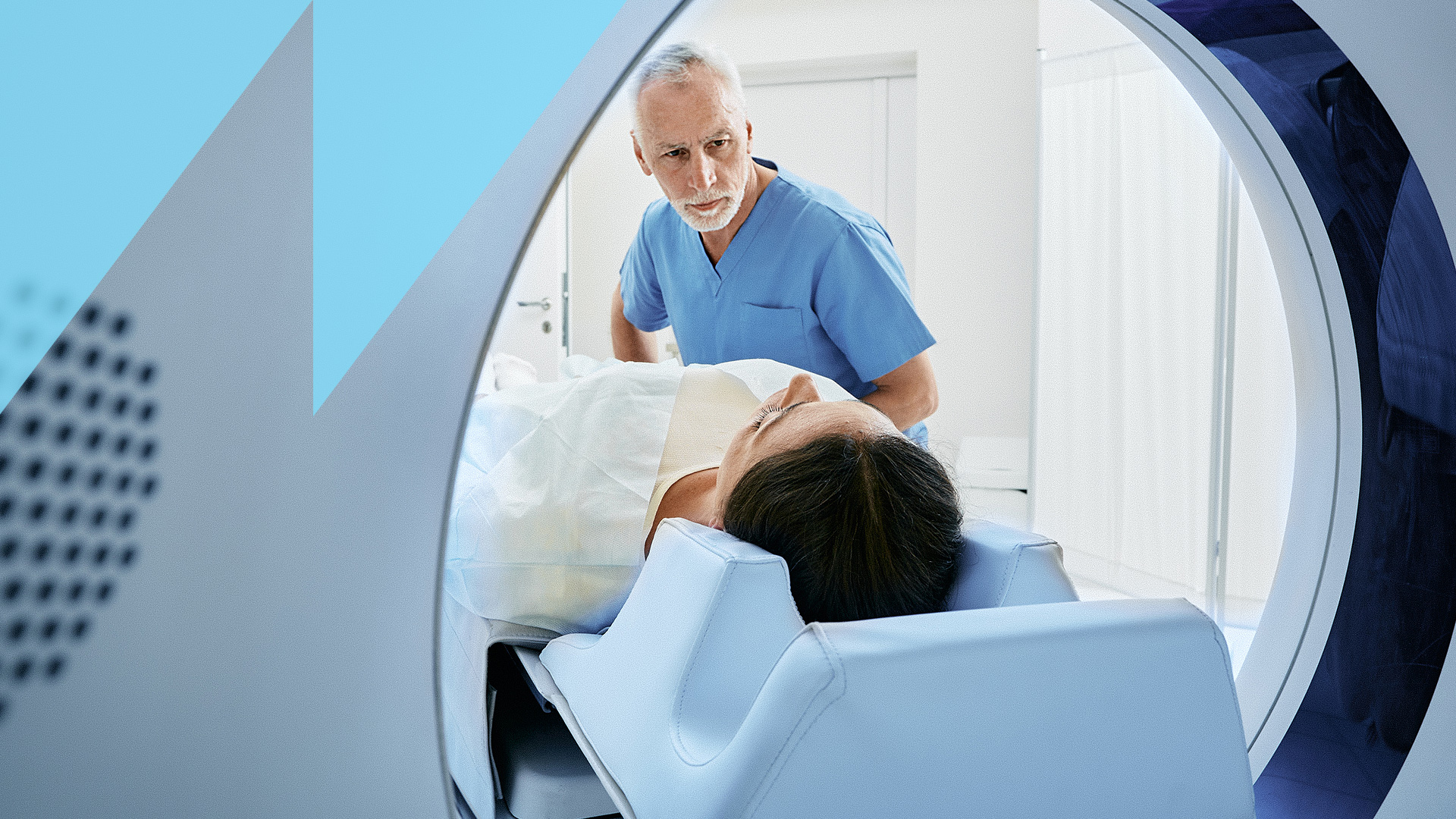
Drawing on SRI’s unique innovation ecosystem, the startup Medical Devices Corner is seeking to improve cancer surgery by advancing MRI-safe teleoperation.
What if you could perform a surgery inside an MRI machine, taking advantage of real-time imaging to locate and destroy tiny sub-centimeter cancer lesions?
That’s the question that animates Sam Frishman, founder of Medical Devices Corner. With support from SRI engineers and advisors, Frishman is building a surgical teleoperation platform that can operate within an MRI machine itself.
“Ten years from now, I truly believe that there will be more minimally invasive surgeries happening inside an MRI than out.” — Sam Frishman
It’s much more complicated than it sounds. Because MRI machines function based on magnetism, common surgical materials — like stainless steel — are off limits. Instead, Frishman is building a surgical system largely out of plastic that leverages hydraulics rather than electricity.
“Ten years from now, I truly believe that there will be more minimally invasive surgeries happening inside an MRI than out,” Frishman predicts. “It will be the gold standard for all kinds of interventions.”
Turning early-stage research into a new healthcare platform
Frishman first became interested in surgical robotics and teleoperation as an undergraduate at Johns Hopkins. There, he found his way to the lab of Professor Dan Stoianovici, who directs the Urology Robotics Program and built one of the first MRI-safe robots. Using air power, the plastic-based system could perform treatments like prostate biopsies and brachytherapy.
“It was a fascinating engineering problem,” says Frishman, “because you can’t have any ferrous metal metals. You can’t use motors. At the time, we were using optical glass fibers instead of wires with electrical current. I worked on some of the newer air-powered motors they were developing.”
Later, while earning his PhD in mechanical engineering at Stanford, he worked on a National Science Foundation grant focused on advancing MRI-safe surgery through hydraulics. That research stemmed from technology developed by the robotics group at Disney Research. He soon joined the Ignite program in Stanford’s Graduate School of Business, developed a venture plan, and founded Medical Devices Corner to further advance MRI-safe teleoperation.
Today, Frishman explains, some brain surgeries already take advantage of MRIs, but those “intraoperative MRI” platforms repeatedly pull a patient in and out of the MRI machine during the surgery. Frishman envisions a more seamless solution.
“[W]e’re building the arms of the system: super-dexterous arms that work inside an MRI machine… It’s really the missing link that opens up the MRI as an interventional suite.” — Sam Frishman
“The way I view this is that you have these amazing eyes into the body, which is the MRI machine,” he says. “Then, between the physician and new AI tools, you have an incredible opportunity to analyze what you’re seeing. And then we’re building the arms of the system: super-dexterous arms that work inside an MRI machine, along with fine needles that can reach organs like the liver, kidneys, the prostate, and the breast, particularly for soft tissue cancer biopsy and ablation. It’s really the missing link that opens up the MRI as an interventional suite.”
The future of surgical teleoperation
Developing from SRI’s Menlo Park labs, Frishman find himself in an ideal place to envision the future of surgical robotics. This, after all, is the same campus that gave birth to Intuitive Surgical, which launched the entire industry of surgical robotics.
One key advantage of the MDC approach, Frishman points out, is that MDC’s ReachMR system will provide surgeons with precise haptic response, enable full-body access, and even compensate for respiratory motion — capabilities not offered by any system currently in the market.
In the next year, MDC will run several pilot studies on the ReachMR system, further refine the platform, and prepare to submit the full system design to the FDA. On this front, he says, hydraulic teleoperation has an unexpected advantage: “Our initial system is fully controlled by the physician. There are no motors, no powered actuation. That really lowers the regulatory barrier, because in some ways, it’s just a very, very fancy scalpel.”
SRI, Frishman emphasizes, has been invaluable as he’s scaled MDC from early prototypes into a platform that is nearing submittal to the FDA.
“We moved to the SRI campus in the summer 2022 and have been building here ever since,” he notes. Along the way, Frishman incorporated SRI-invented visualization technology into his live guidance system and worked with SRI experts to develop a digital twin of the platform. SRI also introduced him to one of the co-founders of Intuitive Surgical, who signed on as an investor and advisor.
While the current platform is focused on soft-tissue cancer biopsy and ablation, Frishman sees an opportunity to expand much further, into MRI-guided cardiac ablations, valve repairs, stroke treatments, and even brain interventions.
“MRI is the best non-invasive imaging method we have,” Frishman concludes. “Unlike a CT scan, there’s no ionizing radiation. Once you have that robot arm, all of the sudden you’re doing all kinds of interventions in the scanner in a way that’s totally safe for the patient.”
Explore how SRI innovations in bioscience and robotics are solving problems and making an impact.